THEMATIC AREA
Infectious diseases in humanitarian contexts
7
pages
What are the main threats to global health security and why?
Infectious diseases represent one of the greatest challenges to public health and global health security, a challenge that has intensified in the twenty-first century. In 2020, the COVID-19 pandemic shook the world, shortly after the major epidemics of SARS, Ebola, Zika, and influenza A. Since then, emerging and re-emerging infectious diseases appear to be on the rise, with outbreaks of cholera, measles, and diphtheria, among others, multiplying.
The two pages in this first section address these threats from complementary angles. One analyses the causes of this global resurgence of infections, the catalysing effect of humanitarian crises, and the rise of antimicrobial resistance. The second examines the response to major public health emergencies of international concern, and preparedness for the next pandemic that will once again threaten global health security.
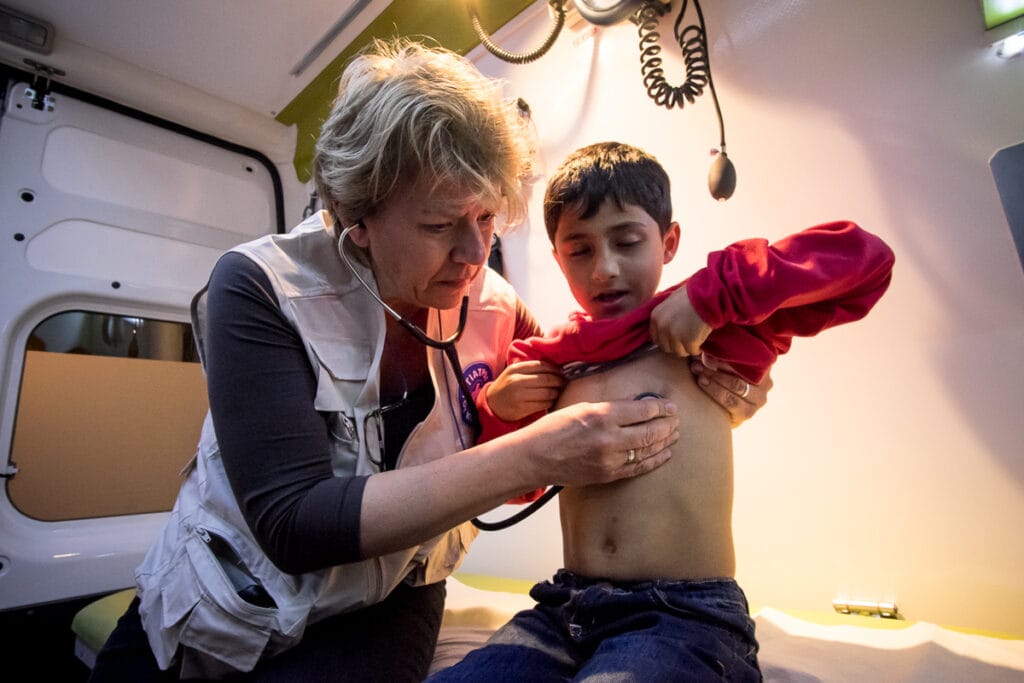
- For the populations most vulnerable to infectious diseases, the threat grows as a result of climate change and the increase in conflicts and forced displacement.
- Humanitarian crises increase the risk of infections, while simultaneously eroding epidemiological surveillance and the capacity to detect and respond to them.
- In 2023, 19 out of 36 countries with a humanitarian response plan experienced an infectious disease outbreak.
- Antimicrobial resistance is an invisible killer in humanitarian contexts. It is estimated that in 2019 it was associated with 4.95 million deaths.
14-minute read + 2 AI-assisted reflection questions
→ Read more.

- Since 2009, the WHO has declared public health emergencies of international concern for influenza A (H1N1), poliomyelitis, Ebola, Zika, COVID-19, and mpox. Each has revealed different weaknesses in global preparedness and response capacity.
- The inequity in access to vaccines, diagnostics, and treatments during the COVID-19 pandemic led the WHO Director-General to speak of a "catastrophic moral failure": one year after a vaccine existed, vaccination coverage was 73% in high-income countries and barely 6% in low-income countries.
- The new Global Pandemic Agreement, adopted in 2025, has been weakened by the concessions and flexibilities required to reach consensus and by the absence of the United States.
15-minute read +1 AI-assisted reflection question
→ Read more.
What are poverty-related infectious diseases and why are they a humanitarian priority?
Poverty-related infectious diseases are those that disproportionately affect people living in overcrowded conditions, with limited access to clean water and sanitation, weak health systems, and nutritional deficiencies that reduce their immune capacity. In humanitarian crises, all these risk factors often intensify simultaneously, turning these diseases into public health emergencies.
The three pages in this section focus on diarrhoeal diseases and cholera, respiratory infections and tuberculosis, and malaria. These are priorities in many situations of poverty, conflict, and displacement, but they are not the only ones. We do not overlook conditions such as polio and measles, covered in the previous section, or HIV/AIDS and sexually transmitted infections, covered within sexual and reproductive health.

- The introduction of oral rehydration therapy in 1979 reduced deaths from diarrhoea in children under five from 4.5 million per year to fewer than 400,000; a much lower figure, but still alarming.
- The majority of deaths from diarrhoea are preventable with access to safe water, sanitation, hygiene, and oral rehydration.
- One of the most dangerous diarrhoeal diseases in humanitarian contexts is cholera, with high epidemic potential.
- Between 2022 and 2024, active cholera outbreaks occurred in more than 40 countries. Cholera vaccination, while useful, should never replace water, sanitation, hygiene, and oral rehydration interventions.
13-minute read + 2 AI-assisted reflection questions
→ Read more.

- Respiratory infections are the leading cause of preventable death in humanitarian and resource-limited contexts. Pneumonia accounts for 14% of all deaths in children under five years of age.
- Tuberculosis kills more than one million people every year and is the leading cause of death in people with HIV. However, it is rarely placed among the priorities of initial humanitarian responses.
- Early diagnosis of tuberculosis is key, but poses an enormous challenge in displaced populations, who are unprotected against the fear of repatriation. Treatment can require up to six months of combined antibiotics, and even longer for its drug-resistant forms.
6-minute read + 1 AI-assisted reflection question
→ Read more.

- Each year, approximately 250 million cases and 600,000 deaths from malaria occur in 85 countries.
- 89% of people in need of humanitarian assistance live in countries where malaria is endemic. Interventions for its prevention, diagnosis, and treatment are complicated by conflicts and emergencies.
- The global malaria eradication effort launched in 1955 failed partly due to overconfidence in technical solutions and partly because sub-Saharan Africa was deliberately excluded, a lesson current strategies cannot afford to ignore.
- Since 2023, two vaccines against malaria have been recommended, but they do not replace vector control or chemoprevention in at-risk populations.
16-minute read + 2 AI-assisted reflection questions
→ Read more.
How are infectious diseases prevented and controlled in humanitarian contexts?
Preventing and controlling infectious diseases in humanitarian crises requires adapting tools that work well in stable contexts to environments where health systems have collapsed or are damaged, where the population is on the move, and where trust in health authorities may be faltering.
The two pages in this final section address the two most important horizontal strategies for doing so: vaccination, and epidemiological surveillance and outbreak response. Both can contribute to preventing and controlling the spread of multiple diseases. Together, they form the foundation for epidemic preparedness and response in humanitarian contexts.

- Since 1974, vaccines have prevented 154 million deaths worldwide, accounting for 40% of the reduction in child mortality during this period. However, every year 13 million children do not receive a single vaccine dose.
- In humanitarian crises, routine vaccination programmes can collapse, precisely when they are most needed. When this occurs, vaccination campaigns are prioritised with reduced schedules for a limited number of antigens, targeting expanded age groups. Deciding which vaccines to prioritise requires careful analysis.
- Initiatives such as Gavi, the Humanitarian Mechanism, and the ICG global vaccine stockpile have improved global access, but inequity in vaccine access remains an unjust and documented reality in every major public health emergency.
12-minute read + 1 AI-assisted reflection question
→ Read more.

- In humanitarian contexts, as the risk of infections increases, the capacity to detect and respond to them deteriorates. When routine epidemiological surveillance collapses, early warning and response systems in emergencies (EWAR) become necessary.
- Epidemiological surveillance enables the detection of signals, which will need to be verified. Analysing their risk makes it possible to decide whether it is necessary to declare an alert and activate a response.
- Experience shows us that responding to an epidemic may require technical control measures, but also appropriate risk communication and community engagement.
10-minute read + 1 AI-assisted reflection question
→ Read more.
Case study: surveillance, vaccination, and epidemic response in humanitarian contexts
Have you read all the pages? Well, I propose an exercise for you to put your knowledge into practice. It consists of a case study with a series of questions. Once you've answered them, press the button for NotebookLM to open. Paste the content of your clipboard there (Ctrl+V on Windows, Command+V on Mac) to get feedback.
🧠 Case study
You work as a health programme manager for an international NGO at an operations base in the north of a sub-Saharan African country. Your team includes two health officers, a WASH officer, an epidemiologist, and a community mobilisation coordinator. You have been supporting primary health services in five health facilities in a district affected by a prolonged conflict for eighteen months, with significant population movements and a camp of approximately 35,000 displaced persons. In the last two weeks, three situations have come to your attention that are causing you concern:
First: the Ministry of Health's EWAR system has recorded an unusual increase in cases of watery diarrhoea in two of the five health facilities you support, concentrated in the northern sector of the camp.
Second: a rapid review of health facility records leads you to suspect low vaccination coverage in the camp, not only for measles but possibly for other vaccines as well. The Ministry of Health, with limited resources, has requested support from humanitarian organisations to plan and implement a vaccination campaign in the camp.
Third: your community mobilisation coordinator informs you that several families in the southern sector of the camp are refusing to attend health facilities. A rumour is circulating that health staff are injecting a substance that causes sterility, apparently linked to a recent vaccination campaign in a neighbouring community.
How do you prioritise these three situations, and what is your first concrete step?
2. Faced with the increase in watery diarrhoea cases recorded by the EWAR, which members of your team would you mobilise to investigate the situation and begin preparing a response plan, and why?
3. The Ministry is requesting support for a vaccination campaign. How would you approach the campaign and how would you prioritise the antigens?
4. The sterilisation rumour is affecting access to services. How do you manage it and what role do you assign to your community mobilisation team?
- 1 Think and write your answer.
- 2 Click on «Copy and open».
- 3 Paste to receive feedback.
📚 This is the NotebookLM of this learning pathway. It uses only carefully selected references. | What is NotebookLM?
Infectious diseases in humanitarian contexts are closely connected to other health priorities. The risk of diarrhoeal infections, for example, is closely linked to child nutrition, HIV/AIDS is a key element in sexual and reproductive health, and all these health problems are addressed through weak or damaged health systems. Furthermore, understanding why these diseases affect people impacted by humanitarian crises so disproportionately also requires a perspective that combines global health and humanitarian health, and that takes into account the lessons of the past from crises such as the Goma cholera outbreak of 1994.
