THEMATIC AREA
Sexual and reproductive health in humanitarian emergencies
Sexual and reproductive rights come under threat in humanitarian crises. This learning resource brings together the normative frameworks, minimum response standards, and key sexual and reproductive health issues affecting populations in emergencies, from gender-based violence to maternal and neonatal health, including contraception, access to safe abortion, and menstrual health. You will find AI-assisted reflection exercises on each page and a case study at the end.
7
pages
Why do reproductive rights matter in humanitarian crises?
In humanitarian emergencies, the sexual and reproductive rights of women and girls can come under severe threat. Gender-based violence surges, access to health services is disrupted, and pre-existing gender inequalities are intensified by the crisis.
Defending these rights is a public health priority from the very first day of the humanitarian response. That is why the sector has adopted a Minimum Initial Service Package for Sexual and Reproductive Health in Crisis Situations (MISP). This first block examines the context that catalysed its publication, the objectives it pursues, the limitations in its implementation, and the impact of the 2025 humanitarian financing crisis.
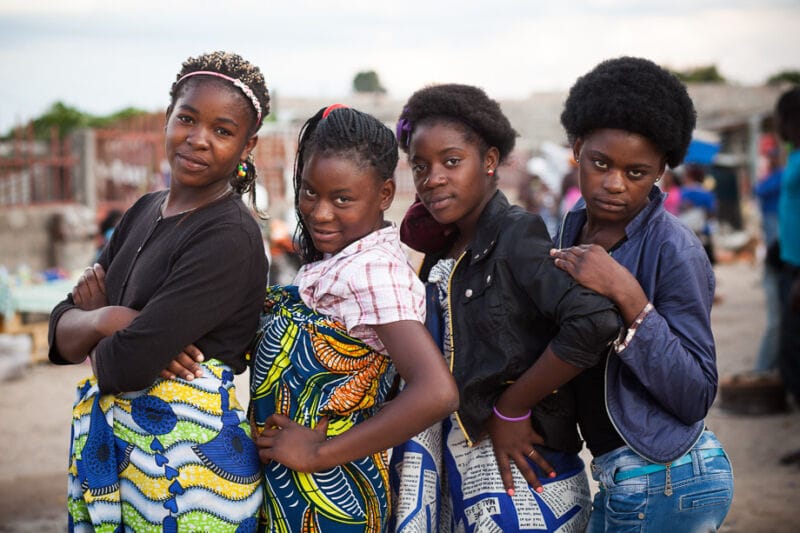
- The 1994 Cairo Conference defined reproductive rights as human rights and highlighted the specific needs of women and girls in humanitarian contexts.
- In response to these needs, the MISP was born, which has been part of the Sphere standards since 2010.
- The MISP is an indispensable minimum designed for the acute phase of an emergency, which should be expanded as it becomes feasible to do so.
- Despite advances, its practical application remains an aspirational goal rather than a reality.
7-minute read + 1 AI-assisted reflection question
→ Read more.
What are the core sexual and reproductive health priorities in conflicts and emergencies?
In contexts of violence, displacement and collapse of essential services, the risk of sexual violence, unwanted pregnancies, sexually transmitted infections and complications during pregnancy and childbirth multiplies. The MISP identifies these as indispensable core priorities.
The four pages in this block explore these priorities in depth, covering the importance, causes and typology of each issue, analysing ways to prevent their causes and address their consequences, and explaining the barriers that exist to protecting the reproductive rights of women and girls in emergencies.

- In conflicts, rape and sexual assault are deliberately used as weapons of war, torture, terrorism and subjugation. In Rwanda, between 100,000 and 250,000 women were raped during three months of genocide in 1994.
- The WHO RESPECT framework proposes seven complementary evidence-based prevention strategies, ranging from the economic empowerment of women to the transformation of gender norms and roles.
- The minimum standards for the response to gender-based violence in humanitarian emergencies include 16 criteria organised around core principles, multisectoral action, and critical coordination and data management processes.
- People who identify as LGBTIQ+ may also face greater discrimination and violence, and encounter additional barriers to accessing assistance and protection services.
14-minute read + 2 AI-assisted reflection questions
→ Read more.

- In conflict-affected areas in Africa, between 43% and 71% of women want to delay or avoid pregnancy, yet it is precisely in humanitarian crises that access to contraception is most difficult and the quality of family planning services suffers most.
- An estimated 218 million women in low- and middle-income countries who do not wish to become pregnant do not use modern contraception. 77% of all unwanted pregnancies occur in this group.
- Ensuring access to modern contraception would reduce unsafe abortions by almost 75% and prevent around 70,000 maternal deaths, among women in low- and middle-income countries alone.
14-minute read + 2 AI-assisted reflection questions
→ Read more.

- In 2023, there were 1.3 million new HIV infections worldwide. Despite advances in diagnosis and treatment, the number of new cases has not declined as expected and prevalence continues to rise in humanitarian contexts.
- Vulnerability to HIV increases in humanitarian emergencies: social protection networks are destroyed, sexual violence increases, access to antiretroviral treatment is disrupted, and food security deteriorates.
- The new global HIV/AIDS strategy 2026-2031 bets on integration into primary care and local leadership. It is a coherent shift from a public health perspective, but one that is happening abruptly in response to the sharp reduction in global funding.
13-minute read + 1 AI-assisted reflection question
→ Read more.
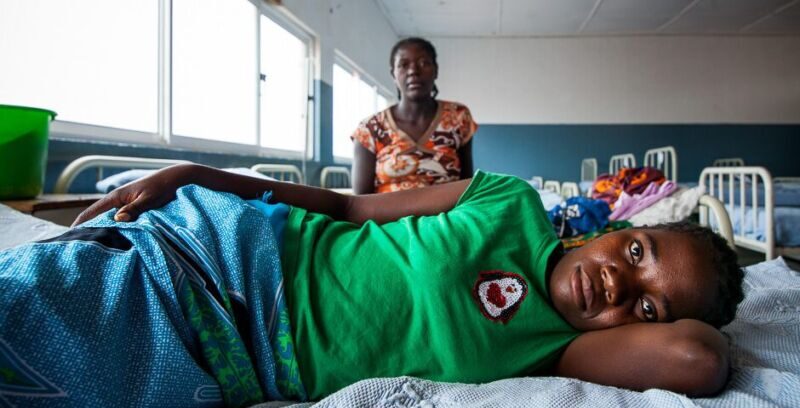
- The maternal mortality rate in humanitarian contexts reaches 504 deaths per 100,000 live births, compared to 11 in high-income countries. Two thirds of all maternal deaths and nearly half of all neonatal deaths occur in humanitarian contexts.
- Most obstetric complications are neither predictable nor preventable. The key lies in their management. This is why emergency obstetric and neonatal care, accessible at community level, is more decisive than antenatal care in reducing maternal mortality.
- The EmONC framework defines care levels with specific essential functions, from managing postpartum hemorrhage to performing a Cesarean section, for example.
- In 2025, the WHO extended the concept of maternal wellbeing to one year after pregnancy, broadening the focus beyond survival.
12 minutes reading + 2 AI-assisted reflection questions
→ Read more.
Which sexual and reproductive health priorities have historically been overlooked in humanitarian action?
Two sexual and reproductive health priorities have historically been sidelined in humanitarian action: access to safe abortion and menstrual health and hygiene. This has been due to political, ideological and cultural reasons that have delayed their recognition and inclusion by decades.
The two pages in this block analyse these resistances, the recent advances that have begun to change them, and what still needs to be done to guarantee these rights to all women and girls in humanitarian crises.

- Every year, 73 million unwanted pregnancies end in induced abortion. 45% of all abortions are unsafe, but this figure exceeds 85% in the countries of central and western Africa, where legal restrictions are most severe. Legal restrictions on abortion do not reduce it: they make it more dangerous.
- For more than two decades after the Cairo Conference, safe abortion care in humanitarian contexts was virtually ignored. Of 11,347 humanitarian projects analysed in a study covering 2002 to 2013, only 13 mentioned abortion care, and exclusively post-abortion care.
- Since 2018, the update to the Inter-Agency Field Manual and the positioning of organisations such as FIGO and MSF have begun to change this picture. MSF went from providing 74 safe abortions in five countries in 2015 to nearly 35,000 in 33 countries in 2021.
9-minute read + 1 AI-assisted reflection question
→ Read more.

- More than one third of people who menstruate worldwide do not have access to adequate materials, sufficient privacy or information to manage their hygiene with dignity. In humanitarian contexts, recent studies show a 34% lack of access to sanitary pads and a 46% lack of access to adequate means of disposal once used.
- It was not until 2017 that the first specific guide was published for integrating menstrual hygiene management into all phases of the humanitarian response.
- The concept of menstrual health, adopted by the Global Menstrual Collective in 2021, broadens the focus beyond materials and infrastructure to include access to information, care for menstrual disorders, and addressing stigma and discrimination, including trans men and non-binary people who also menstruate.
- In 2026, menstruation remains a marginal issue on the agendas of organisations such as UN Women and UNFPA, and is absent from the Sustainable Development Goals.
9-minute read + 1 AI-assisted reflection question
→ Read more.
Case study: reproductive rights and forced displacement
Have you read all the pages? Well, I propose an exercise for you to put your knowledge into practice. It consists of a case study with a series of questions. Once you've answered them, press the button for NotebookLM to open. Paste the content of your clipboard there (Ctrl+V on Windows, Command+V on Mac) to get feedback.
🧠 Case study
Nagina is 32 years old and has been living for six weeks in a camp for internally displaced persons after a flood destroyed her village. She lives in a tent with her husband, her youngest child, a four-year-old boy, and her eldest daughter, aged 12. Her other two daughters are staying with relatives in another region; she has not seen them since arriving at the camp.
The camp is overcrowded. Nagina only leaves the tent when absolutely necessary: she has seen women fight with unknown men at food distribution points. Her husband turned down a job because he did not want to leave her alone. In recent days he has told her he does not want her to go out alone or with women he does not know.
Nagina believes she is four months pregnant. She has not told anyone. She has had no antenatal care since arriving at the camp and does not know where she would be able to give birth. She does not want this pregnancy: she already has five children, the family has no income, and the atmosphere in the tent is deteriorating by the day. She has thought about terminating it, something that would be legal in the country where she is, but does not dare speak to anyone about it, not even the staff at the health post, which she has never visited on her own.
Her 12-year-old daughter had her first period three weeks ago, just after arriving at the camp. Nobody had explained to her what it was. She has severe cramps and there are no painkillers or sanitary pads available in the tent. Neither she nor Nagina dare raise this problem with her husband.
1. What gender-based violence risks do you identify in Nagina's situation, and what factors at the individual, community and social level explain them?
2. What other sexual and reproductive health needs do Nagina and her daughter have beyond gender-based violence, and how are they interrelated?
3. If you are part of the camp health team, how do you think these services should be designed so that people like Nagina feel safe enough to talk about their needs?
4. What services should the camp guarantee to cover the needs you have identified, and which would be most difficult to implement at this stage of the emergency?
- 1 Think and write your answer.
- 2 Click on «Copy and open».
- 3 Paste to receive feedback.
📚 This is the NotebookLM of this learning pathway. It uses only carefully selected references. | What is NotebookLM?
Nagina's situation cannot be understood solely through the lens of a technical sector and its sexual and reproductive health subsector. All these services are embedded within a health system and depend on its strength and functional capacity, while at the same time connecting with other priorities, such as malnutrition during pregnancy and the risks of prematurity and low birth weight, for example. They must also be closely interconnected with psychosocial support and mental health, the mainstreaming of protection approaches, and a necessary gender perspective integrated throughout the programme cycle and the organisational culture of humanitarian actors.
